Explore this article:
- What is Fascia?
- How to Unlock Fascial Tension
- Understanding Fascial Inflammation
- DIY Myofascial Release
If you could peek beneath your epidermis, you’d first see fascia — a messy, white, elastic tissue made of collagen fibers, similar to the material making up your ligaments and tendons. The meshlike substance interweaves through and around your musculature and bones, supports your organs, and shrink-wraps your entire internal structure like a second skin.
In the past, fascia was out of sight, out of mind. “From an anatomical perspective, fascia is often seen as ‘the gunk you cut through to get to the good stuff,’” says corrective-exercise specialist Anthony Carey, MA, CSCS, of Function First in San Diego.
In recent years, however, trainers, physical therapists, athletes, and everyday exercisers have begun to understand that this seemingly inconsequential webbing plays an important functional role.
Experts are now devising ways to improve the quality and elasticity of the fascia through bodywork, stretches, and targeted exercises, building on ideas outlined by bodyworker Thomas Myers in his book Anatomy Trains: Myofascial Meridians for Manual and Movement Therapists. These methods can significantly enhance the benefits of a stretching and strength program, helping you stand taller, run faster, and move better.
At the same time, bodywork focused on the muscle–fascia (myofascial) connection often provides relief from chronic back and joint pain when conventional, muscle-based stretching and massage methods fail.
“Everybody needs to start incorporating the fascia into their conception of the musculoskeletal system,” Myers says. And this signals a substantial shift in the way we think about how we’re made and how we move.
What is Fascia?
Anatomy textbooks tell us that the musculoskeletal system consists of thousands of parts: a couple hundred bones held together by more than 600 muscles and numerous ligaments and tendons. But experts now assert that these divisions are largely artificial, created not by nature but by anatomists.
“The fascia links the entire muscular system, not just muscle to bone but muscle to muscle, along with all the structures in the body, like organs, ligaments, and tendons,” explains Carey. “Whether you’re exercising or treating pain, it doesn’t make sense to treat it like a machine with separate parts, because of this head-to-toe continuity.”
Seen from this perspective, Myers contends, “You don’t have 600-some-odd muscles, as we’ve always been taught: You have a single muscle in 600 fascial pockets: one mind, one muscle, one fascial web.”
Far from the haphazard mesh that earlier anatomists perceived, this fascial network is now described as sensitive, dynamic, and extraordinarily adaptable. “There are 10 times as many nerve endings in your fascia as there are in your muscles,” says Myers; this makes fascia far more susceptible to pain and sensation than your muscles. “Most sports injuries are in fact failures of fascial structures, not muscle tissue.
“We say muscles attach to bones, but muscle can’t attach to anything. It’s formless, like hamburger. It’s the fascia that goes over and around and through your muscles that organizes that tissue into linear pulling machines.”
“We say muscles attach to bones, but muscle can’t attach to anything. It’s formless, like hamburger. It’s the fascia that goes over and around and through your muscles that organizes that tissue into linear pulling machines.”
When you perform a biceps curl, for example, the fascia of the biceps muscle shortens, tugging on your tendons and drawing your hand closer to your shoulder. And when you do a quick, athletic movement — a lay-up in basketball, for instance — it’s the whip-fast elastic action of the fascia in your legs that transfers the force of those contracting muscles into the floor and launches you off the hardwood.
The webbing is organized into what Myers calls myofascial meridians, or trains — distinct, dense bands of fascia. These bands connect multiple muscles and span multiple joints; they are tacked down at numerous bony points along the way.
There are about a dozen of these myofascial bands. Some run the length of your body, head to toe; others spiral the torso, shoot over the top of your head, and run down the middle of your back.
A balanced, harmonious tension among these myofascial bands helps support fluid, effortless movement. Too much chronic tension or slack in key meridians can lead to poor posture, as well as pain — and not always in the places you expect.
Trace the bands through the muscles and across the skeleton, and it’s possible to see, for instance, how shoulder pain might be caused by dysfunction in your opposite ankle, or how tight hamstrings might actually be caused by tension in the soles of the feet.
“Fascia adapts to every move you make — good, bad, or indifferent.”
It’s through these myofascial bands, more than through individual muscles, that the body adapts to and reinforces alignment and movement. “Fascia adapts to every move you make — good, bad, or indifferent,” explains Carey.
Over time, a competitive rower, for example, might develop thick fascia in her back and shoulders to support the movement of pulling oars. The fascia in the front of the rib cage of your typical desk jockey, on the other hand, may thicken and shorten to reinforce a habitually caved-in posture.
And injuries, even minor ones, often result in myofascial “patches” in the muscles that can restrict motion, leading to compensations in gait and movement. These might remain long after the injury itself has healed.
“Injured or poorly adapted fascia can start to act like glue, binding to muscles, other fascia, even your ligaments,” Carey says. Your life history — exercise habits, injuries, common sitting and sleeping positions — becomes formed into your fascia.
Depending on these and other behavioral factors, myofascial adhesions can subtly accrue over time, leading to movement inhibition and sometimes chronic pain.
“Certain things in our bodies become tight, certain things become weak, and before you know it, our joints and limbs begin to make subtle twists and turns, making us a human game of Jenga.”
“Certain things in our bodies become tight, certain things become weak, and before you know it, our joints and limbs begin to make subtle twists and turns, making us a human game of Jenga,” jokes physical therapist Sue Falsone, MS, PT, SCS, founder of Structure and Function, a Phoenix-based firm that uses dry needling for myofascial rehabilitation.
Fascia is “the glue that connects everything,” and the quality of that glue can help support mobility and unrestricted movement — or it can get us stuck in limited, uncomfortable, or painful patterns, explains Debbie Lensing, DPT, OCS, Cert-DN, a physical therapist at Life Time’s LifeClinic in Chanhassen, Minn.
“Injuries, or years of poor posture and poor movement patterns, can create a snowball effect of affecting not only the original restricted joint or tissue but also the joints and tissues above and below the original area,” Lensing says. Working on mobility in the muscles and joints can help “unstick” the fascia and maintain normal fascial mobility.
How to Release Fascial Tension
If you gravitate toward exercise when your fascia feels full of kinks, you’re on the right track. “Muscles and fascia are so interwoven that you can’t affect one without affecting the other,” Falsone says.
But intermittent activity and static stretching has little effect on deeply ingrained fascial tension — especially if, like many people, you regularly sit for long periods of time.
“If we spend months, years, even decades sitting at a desk and think that a few hours in the gym per week are going to undo all that, we’re probably fooling ourselves,” says Carey. Stretching a muscle with bound-up or poorly adapted fascia is a bit like trying to stretch a knotted bungee cord: You’ll get much better results if you untie the knots first.
That may require working with a practitioner while lying on a massage-style table. Acute fascia issues, which can take the form of chronic pain and immobility, are particularly responsive to table work, which may involve your active participation.
“Table work helps a client find more pliability and elasticity throughout the body,” explains Carey. “Exercises help the client integrate the new range into their daily lives.”
Whether you choose to work with a qualified therapist or not, you can try these movement patterns on your own:
Full-body movements:
Rather than trying to build or use different body parts in isolation, working with implements like battle ropes, Indian clubs, and kettlebells can address some imbalances. Olympic lifts and medicine-ball throws can be helpful, as well.
Many of these movements require a dynamic transfer of force from the ground, through the body, and out through the arms or hands — a pattern that simulates a wave. Done correctly, these wavelike motions mimic the sequential, muscle-to-muscle transfer of force that occurs along the fascial meridians just below the skin. These can help reinforce healthy, integrated relationships among the bands.
Multiple-plane mobilizations:
Rather than stretching one muscle group at a time, try stretching an entire plane of the body at once and performing long movements that extend and spiral the body from head to toe. Add rotation of the feet to a toe-touching stretch, for example, in order to fully extend the fascia across the hamstrings, calves, and lower back. The asanas in yoga and the gentle oscillations of the Feldenkrais Method are good examples of fascia-releasing work that enhances flexibility.
Bounces:
For greater suppleness through the fascia, incorporate bouncing in your workouts — think skipping rope, jogging, jumping on a trampoline. “You lose elasticity in your fascia as you age. Kids exemplify that bouncy elasticity in their fascia, and bouncing helps you hold on to what you have,” explains Myers.
Diverse movements:
Variety may be your best safeguard against fascial tightness and adhesions, Myers notes. “If there’s one thing I could say to people who wanted to get fit or stay fit, it would be, ‘Stop repeating yourself!’”
Repetitive physical action — including running and cycling — can leave its mark on the fascia, unnaturally tightening certain areas and eventually leaving you more susceptible to injury. So mix things up. Cycle or hike on uneven terrain, switch strength-training exercises frequently, and seek out new ways to move, through dance, sports, martial arts, or other activities.
Integrated exercises:
Progressive fitness professionals are now emphasizing integrated forms of exercise, including dynamic flexibility work, full-body strength training, outdoor exercise, and mindful movement, such as tai chi. Just as the fascia interconnects the muscles physically, integrated exercise and movement link the muscles functionally through dynamic, coordinated movement patterns.
“Fascia is not a new tissue, just a new point of attention,” explains Myers. More than just an underrecognized contributor to movement and joint health, “the fascia regulates the body’s biomechanical reality.” Like the body’s other systems, it’s both active and reactive, acting upon and responding to your internal and external environments. “The new point of view profoundly changes how we go about training — from the ground up.”
The more we can shift our perspective to see the body as a whole system working together, the healthier we’ll be.
Understanding Fascial Inflammation
Long-term inflammation and irritation in the fascia are fairly common — and can sometimes aggravate certain arthritic conditions.
What causes fascial inflammation? “No one knows for sure. It’s partly genetic, but it’s often related to overdoing one particular type of movement,” says Nadine Samila, a Calgary, Alberta–based practitioner of Anatomy Trains Structural Integration and Myofascial Release Therapy (MRT).
Inflammation and tightness in the iliotibial, or IT, band (the thick fascial strap that runs along the outside of your thigh), for example, is common in runners. “A tight IT band can pull the kneecap off its track, which irritates the knee joint and can eventually lead to arthritis,” says Chris Frederick, PT, coauthor of Stretch to Win.
Perhaps the worst myofascial inflammation is compartment syndrome, a restriction of the fascia surrounding lower-leg muscles that often afflicts overtrained athletes.
Still, it’s plain old inactivity that causes most myofascial troubles. Desk-sitters will often struggle to reach behind themselves comfortably from a seated position because the fascia in and around their pectoral muscles constricts. As a result, the smaller, weaker muscles of the rotator cuff can get strained or injured, even during seemingly harmless movements. “I’ve had clients who have torn their rotator cuffs trying to reach something in the back seat of their car,” says Frederick.
Similarly, habitual slumping and slouching can cause the fascia in the chest to shorten and tighten, restricting freedom of movement in the arms and shoulders.
Healthy fascia is well hydrated and smooth, like the fine membrane that covers fresh, uncooked chicken. But the connective tissue in older and inactive people “gets fuzzy and sticky, like cobwebs,” explains Samila. “It doesn’t move well. That’s partly due to age, but inactivity makes it much worse. We just don’t move enough!”
The antidote?
Move. As much as you can, and in as many different ways as possible.
“The more you move, and the more ways that you move, the more you keep the fascia soft, hydrated, and healthy,” Samila says.
DIY Myofascial Release
Try some of the following exercises to ease tension. Activities that include long and sweeping patterns, full extension of the limbs, and spiraling gestures through the torso (notably yoga, tai chi, and Feldenkrais) can enhance awareness and foster optimum balance of your body’s major myofascial bands. Many dance styles, as well as racquet sports and ball sports, which require jumping, leaping, throwing, and reaching, have similar benefits.
“The Worlds Greatest Stretch”
This stretch, recommended by Sue Falsone, MS, PT, SCS, mobilizes myofascial bands in the front of the hips as well as the back of the body, head to toe.
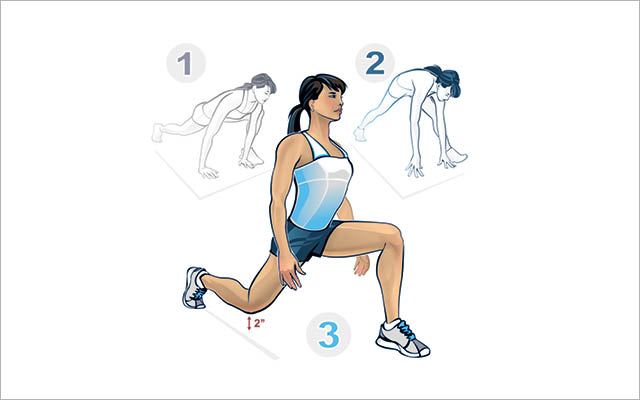
- Stand and step forward with your left foot into a deep lunge position. Lean forward and place both hands on the floor, with your left knee outside your left arm and shoulder. Keeping your right leg straight and your back long (aim for a perfect line between your head and right heel), gently press your left elbow against the inside of your left knee for a two-count.
- Keeping your right leg fully extended, slowly straighten your left leg as much as possible, rocking your weight back onto the heel of your front foot. Hold for a two-count.
- Rebend your left knee and lift your torso from the bent-over position, assuming a high lunge position with your right knee floating 2 inches off the floor. Hold for a two-count, then step forward with your right foot and repeat on the opposite side. Perform six to eight repetitions on each side.
Side Bend With Rolling Feet
Although the standard side bend has traditionally been used as a stretch for the lats and obliques (the muscles on the sides of your torso), rolling the feet in this position — which inevitably intensifies the stretch — extends a unified fascial band along the side of the body from the outside edges of your feet all the way up to your ear.
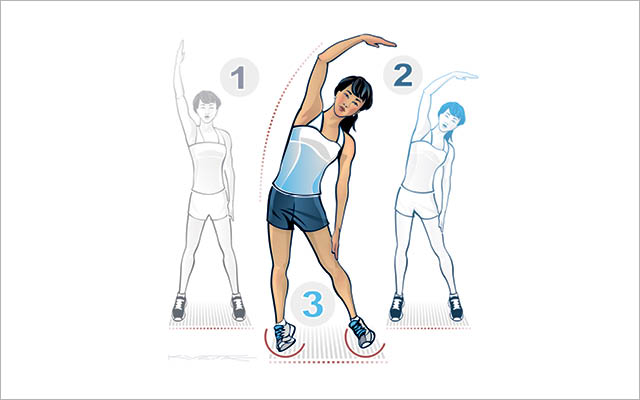
- Stand upright with your feet parallel and just over shoulder width apart. Keeping your hips and shoulders square, reach your right hand directly overhead.
- Perform a side-bend to your left, reaching your right arm over your head and as far to your left as possible.
- Once in this position, roll both feet to the right, shifting your weight onto the outside edge of your right foot and the inside edge of your left foot. Hold for 10 seconds and repeat on the opposite side.
A Better Hip Mobilization
Many people stretch their hips and hamstrings in one plane of motion — straight forward (as in touching your toes). Because the fascia runs through and around the entire musculature, try instead stretching in a multiplanar way: up, down, forward, back. Avoid the pain threshold; if your body feels pain, the protective mechanisms of your joints will tighten and shorten muscles as you stretch.
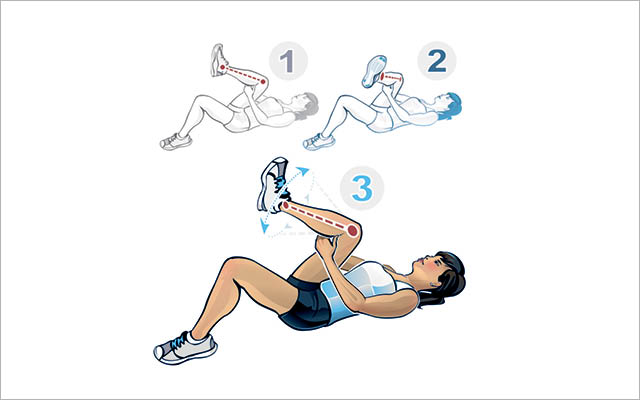
- Lie flat on your back on a firm surface. Bend both knees with feet flat on the floor. Lift your right leg in the air and take hold of your leg with both hands — behind your knee, on the outsides of your thigh, or wherever feels comfortable.
- Keeping your neck relaxed and your head on the floor, gently pull your leg toward your upper body until you feel a gentle stretch.
- Maintaining your hold on the leg, gently rotate your foot, circling your leg to the outside, then to the inside of your torso. Continue to experiment with easy movements of your leg, in whatever range and plane of motion feels comfortable, for about two minutes; then repeat on the other side.
Tennis Ball Rollout
Rolling out the bottoms of your feet on a tennis or other type of ball will loosen the fascial band that runs from there to your head.
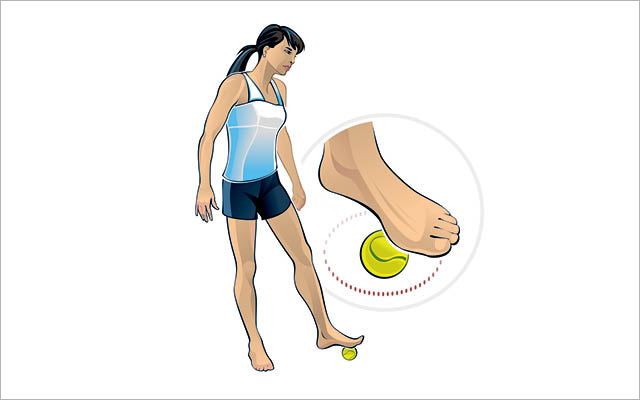
- Before you start, perform a standing toe-touch in bare feet, with your knees soft, and note how far you can reach without straining.
- Now, stand tall and carefully roll the bottom of one foot over a tennis ball, paying particular attention to spots where your foot is tender or sensitive.
- Hold on to something stable for balance if necessary.
- Continue for at least one minute, then repeat on the other foot.
- Repeat the standing toe-touch test and note how much farther you can reach.
This originally appeared as “The Web of Life” in the November 2011 print issue of Experience Life.



This Post Has One Comment
The myofacial article was written very well and very informative. Thank you for making it available!