There are few parts of a geezer’s anatomy that get as much surgical attention as our creaky knees. U.S surgeons perform about 700,000 knee-replacement procedures every year, making it America’s most popular elective surgery. It may also be the only operation whose results depend more on your insurance coverage than your surgeon’s skills.
Boston University researchers last week released the results of a study revealing that patients covered by private insurance experienced fewer postsurgical complications than those covered by Medicare — and it wasn’t even close.
When adjusted for age, sex, and other demographic factors, Medicare patients were more than twice as likely as their privately insured peers to suffer a “cardiac event” as a result of the surgery and nearly twice as likely to contract a urinary-tract infection. Among the other complications that tended to strike the Medicare set more often than the privately insured were central-nervous-system problems, gastrointestinal troubles, wound breakdown, and postoperative anemia. Not surprisingly, mortality rates among those with Medicare coverage were also higher.
The study, published in the journal Orthopedics, corroborated earlier research findings. The authors did not, however, offer any clues as to why such disparities would occur, noting only that further research would be needed. “As the landscape of healthcare changes with both reimbursements and bundle payments for joint arthroplasties,” study coauthor Xinning Li, MD, noted, “insurance status or patients with lower socioeconomic status should be factored into the final formula and risk adjusted for both physician and hospital reimbursement.”
Medicare tends to pay less than private insurers for procedures, so a cynic might conclude from the evidence that the quality of care in these cases may have something to do with the quantity of dough that ends up in the surgeon’s pocket. Far be it for me to suggest such a thing, though. I’ll leave that up to Duke University physician and behavioral scientist Peter Ubel, MD.
Writing in Forbes, Ubel argues that Medicare’s attempts to lower knee-replacement costs and improve outcomes through a new “bundled payments” initiative may lead to surgical decisions that don’t necessarily benefit the patient. The new reimbursement plan, he explains, offers a lump sum to the healthcare facility to cover everything from the surgery to postop physical therapy rather than sending separate payments to each service provider. As a result, surgeons earn less money per operation and may be tempted to perform more surgeries to maintain their income. Some portion of those additional operations, he notes, may involve patients who are not necessarily prime candidates for the procedure — potentially leading to poor postop outcomes.
(Spare your tears for the aggrieved orthopedic surgeon; your average knee-replacer scrapes by on $463,731 per year, according to a recent survey.)
“I’m not suggesting that surgeons will purposely perform unwarranted procedures. I’m certainly not implying that they will put artificial knees in people who have little or no knee trouble,” Ubel writes. “Medical practice is often about making tough judgment calls. And I worry when people’s incomes start declining, it will subtly influence their judgment.”
To be fair, early evidence has not revealed a tsunami of what a cynic might call “income-replacement” surgeries. Hospitals that have enrolled in the bundled-payments plan report performing only a handful of additional knee-replacement operations under the program. Procedures at hospitals not participating in the plan, however, have remained stable. Still, Ubel warns, “All these findings are tremendously preliminary. Bundled payments are still in their infancy. Quality measurement still doesn’t capture everything we’d like it to.”
And hospitals are not the most transparent institutions. A recent report out of Washington University School of Medicine found that about a third of the 1,010 U.S. hospitals that researchers surveyed did not provide Medicare-mandated quality-of-care data — despite receiving hefty fines for not responding. The study’s authors suggest that the reporting process may have been too much of a burden for some organizations, which certainly may have been a factor. But those facilities that did report tended to demonstrate higher-quality care, which might cause a cynic to wonder whether those less-forthcoming hospital administrators simply had nothing positive to declare.
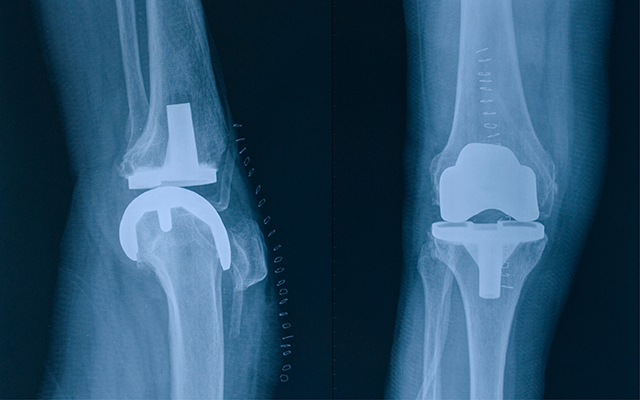
I’m fortunate to be operating with two mostly functional knees, so I don’t spend any time considering whether I should pay someone to slice them open, rip out the malfunctioning joint, and insert some ingenious metal-and-plastic mechanism in its place, which may possibly become infected, fall prey to an immune-system attack, or simply damage nerves and blood vessels — all leading to additional surgery. Then, if by chance all goes well, do it all over again in my 80s (the artificial joints last only 10 to 15 years on average).
But that’s probably just me.
And it frankly feels a bit silly to contemplate surgical procedures while observing My Lovely Wife’s 40-year conversation with her bum right knee, which she injured in a freak accident that 1970s state-of-the-art orthopedic surgery remedied by removing all its cartilage. She has gradually adapted to her recalcitrant joint’s frequent complaints by studying Feldenkrais, practicing yoga, pedaling her bicycle, and generally moving with the sort of mindfulness that I only dream of achieving.
We are clearly a couple of outliers here in Geezerville. The American Academy of Orthopaedic Surgeons estimates that the number of primary, or first-time, knee replacements will grow by 189 percent by 2030. Revisions — replacing the joint for the second time — will increase at a slightly higher rate. If those projections prove accurate it’ll mean my peers on Medicare will continue to flood hospitals seeking a magical remedy for their creaky knees — despite the many risks — and our struggling orthopedic surgeons won’t ever have to worry about making their mortgage payments.
This Post Has 0 Comments